Key takeaways:
- Pain is not just a physical sensation but a multidimensional experience shaped by emotions, thoughts, and social factors.
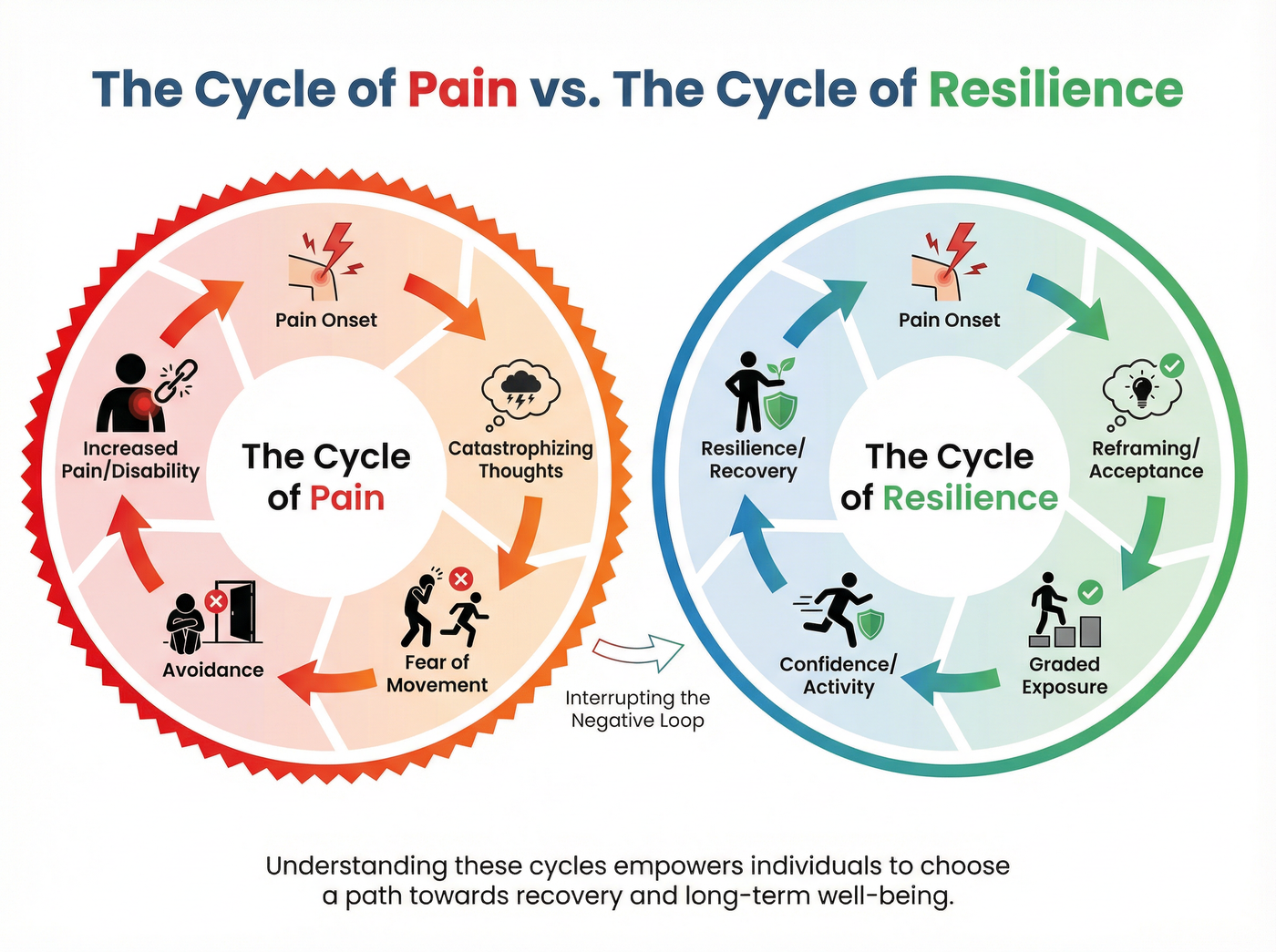
- Catastrophizing—focusing on the worst possible outcome—can amplify pain signals and lead to a vicious cycle of disability.
- Resilience is a dynamic, trainable skill, not a fixed personality trait.
- Psychological interventions like cognitive reframing and mindfulness can physically alter brain structure and improve pain outcomes.
We often think of pain as a simple alarm system: you touch a hot stove, and your brain signals "danger." The assumption is that the pain is directly proportional to the physical damage. However, as explored in the Pody.fm episode The Science of Pain: Resilience That Fuels Progress, this traditional view overlooks the profound complexity of human suffering. Host Josh Bowman and expert Nash Daniel delve into the science revealing that pain is a "multidimensional nature"—a constructed experience that we can influence.
Beyond Tissue Damage: The Biopsychosocial Model
The International Association for the Study of Pain (IASP) defines pain as an unpleasant sensory and emotional experience associated with actual or potential tissue damage. This definition highlights that pain is subjective. While acute pain protects us by prompting rest and healing, chronic pain often persists long after tissues have healed.
Modern research supports a biopsychosocial perspective. This model posits that our experience of pain is the result of intricate interactions between biological factors (genetics, injury), psychological factors (mood, trauma, beliefs), and social factors (support systems, culture)[2]. Understanding this interplay explains why two people with similar injuries can experience vastly different levels of suffering—and why fixing the physical problem doesn’t always stop the pain.
The Trap of Catastrophizing
One of the most significant psychological barriers to recovery is catastrophizing. This cognitive pattern involves ruminating on pain, magnifying its threat, and feeling helpless to control it. Catastrophizing acts as an amplifier; it increases anxiety and hypervigilance, which in turn sensitizes the nervous system to feel more pain[3].
Researchers have identified that reducing catastrophic thinking is a primary mechanism through which psychological interventions succeed. By breaking the cycle of fear and avoidance, individuals can lower their pain perception and regain physical function[3].
Resilience: A Skill, Not a Trait
A hopeful revelation from recent neurocognitive findings is that resilience is not a static trait you are born with. Instead, it is a dynamic process that fluctuates based on your emotional state, mindset, and coping strategies. This "neurocognitive process" involves specific brain regions responsible for emotional regulation and executive control[8].
Neuroscience has even pinpointed structural differences in the brains of resilient individuals. A 2025 study highlighted that lower gray matter volume in brain regions associated with cognitive and affective stability is a risk factor for poor pain outcomes[7]. Theories like Acceptance and Commitment Therapy (ACT) and Cognitive Behavioral Therapy (CBT) leverage the brain's neuroplasticity. By changing how we process thoughts and emotions, we can literally reshape our neural architecture to become more resilient to pain.
Reframing the Experience
Transitioning from a mindset of helplessness to one of growth requires active "cognitive reframing." This involves identifying distorted, negative thoughts and challenging them with evidence-based, balanced perspectives[5]. This shift isn't about ignoring pain but viewing it as a temporary challenge rather than a permanent state of damage.
Below is a comparison of how different mindsets influence the pain experience:
Comparing Mindsets in Pain Management
| Feature | Catastrophizing Mindset | Resilient/Growth Mindset |
|---|---|---|
| Focus | Focuses on the threat and "worst-case" scenarios. | Focuses on adaptability and problem-solving. |
| Reaction to Pain | Avoidance of movement (fear-avoidance). | Gradual engagement (exposure) despite discomfort. |
| Emotional State | Helplessness, anxiety, and distress. | Acceptance, self-compassion, and perseverance. |
| Outcome | Increased disability and pain intensity[1]. | improved physical functioning and lower distress[8]. |
Steps to Fuel Progress
To cultivate resilience, experts recommend shifting focus from solely eliminating pain to improving quality of life. Strategies include:
- Education: Understanding that "hurt does not equal harm" can reduce the fear associated with movement.
- Exposure in Vivo: Gradually confronting feared activities can prove to the brain that movement is safe, reducing the fear-avoidance response.
- Social Connection: Building robust support systems creates a "ripple effect," where shared stories of perseverance inspire collective strength[1].
- Positive Affect: Cultivating positive emotions—even in small doses—can buffer against the stress of chronic pain[4].

Ultimately, pain demands attention, but it doesn't have to dictate your life's limits. By understanding the science behind your mind and body, you can turn a painful struggle into a profound journey of growth.
Listen to the episode
Dive deeper into the conversation with Josh Bowman and Nash Daniel on how to unlock your potential for resilience.
Listen to The Science of Pain: Resilience That Fuels Progress
Sources
- Reframing pain: the power of individual and societal factors to enhance pain treatment (PAIN Reports)
- Reframing pain: the power of individual and societal factors to enhance pain treatment (PMC)
- Psychological Interventions in Patients with Physical Pain: A Focus on Catastrophizing and Resilience
- Pain is Temporary, Growth is Permanent: Navigating Short-Term Struggles for Long-Term Strength
- Shift Your Perspective, Transform Your Life: Cognitive Reframing Techniques That Work
- Pain resilience dimensions and regional gray matter volume as risk factors for poor outcomes of chronic pain
- Reviewing Psychological Practices to Enhance the Psychological Resilience Process for Individuals with Chronic Pain
