For decades, the placebo effect was dismissed by scientists as a “nuisance variable”—a statistical ghost that researchers had to exorcise to determine if a new drug actually worked. Today, however, neuroscience is flipping that script. We now understand that the placebo effect is not merely an imaginary trick; it is a profound biological capability of the human brain to regulate the body's internal states.
Listen to the episode
From Battlefield Desperation to Clinical Breakthrough
The story of the modern placebo effect begins in the chaos of World War II. Dr. Henry Beecher, an anesthesiologist serving as a medic, faced a nightmare scenario: a critical shortage of morphine with wounded soldiers screaming in pain.
Out of options, one of the nurses injected a soldier with simple saline solution but told him it was morphine. Astonishingly, the soldier settled down and reported significant pain relief. This observation led Beecher to publish his landmark 1955 paper, The Powerful Placebo, in which he estimated that approximately 35% of patients could achieve effective clinical relief solely based on their belief in the treatment.[5]
Mapping the “Internal Pharmacy”
While Beecher observed the effect, modern technology has allowed us to see it. Research confirms that the placebo effect is not “all in your head” in a figurative sense, but rather rooted deeply in your brain's anatomy. It is a genuine physical process.
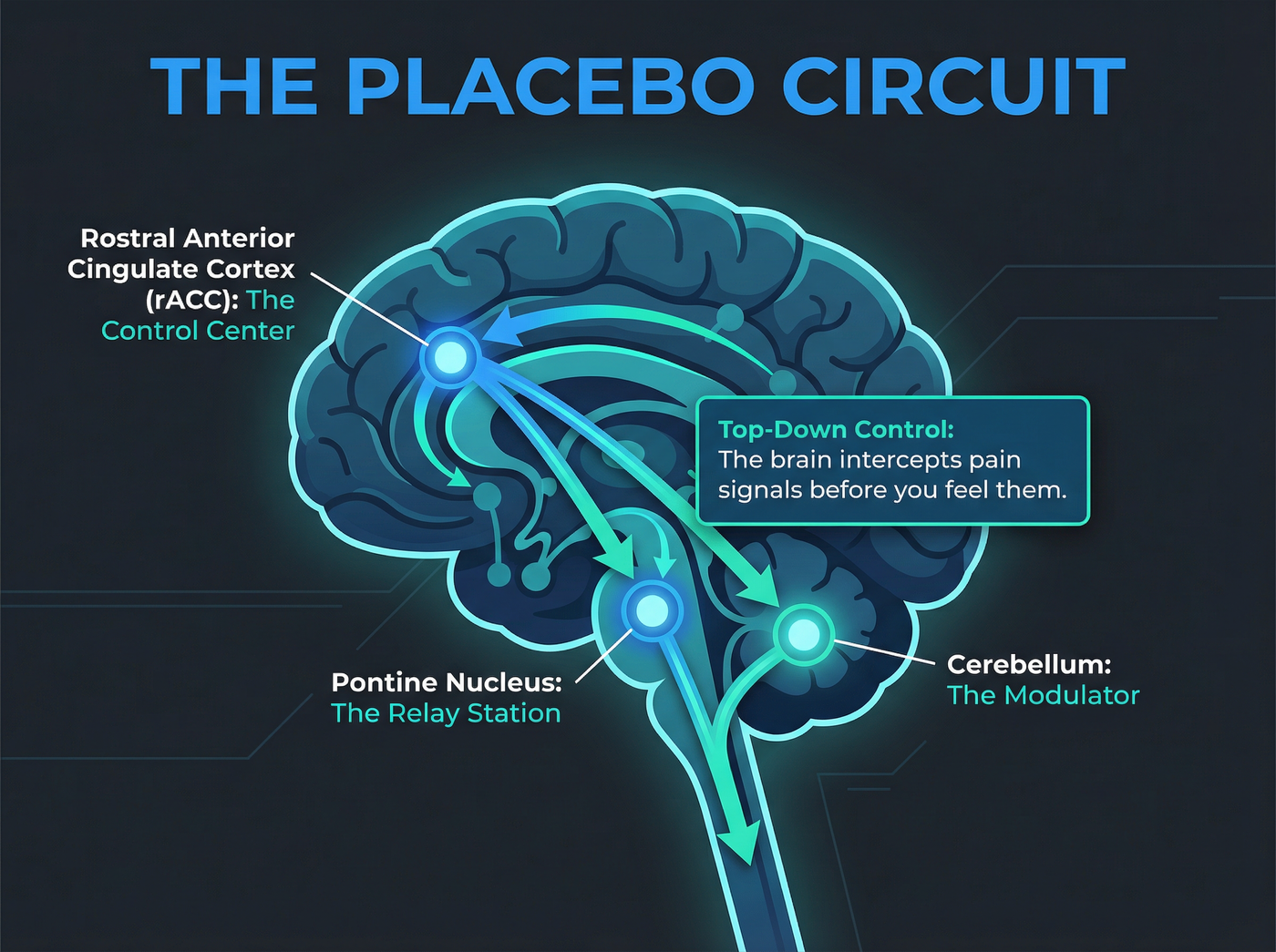
Scientists have mapped a distinct “placebo circuit” that acts as a top-down control mechanism for pain. This pathway originates in the rostral anterior cingulate cortex (rACC), a brain region involved in emotion and cognition. From there, signals travel to the pontine nucleus and finally to the cerebellum.[1]
This neural route is densely populated with opioid receptors. When a patient anticipates relief, the brain releases its own natural painkillers (endorphins) through this circuit, intercepting pain signals before they reach conscious awareness.[3] This effectively means the brain functions as its own internal pharmacy, dispensing chemical relief based on expectation.
Honesty is the Best Medicine: Open-Label Placebos
Perhaps the most mind-bending discovery in recent years is that deception is not required for the placebo effect to work. For a long time, it was assumed that patients had to believe they were getting real medicine.
However, open-label placebo studies have shattered this assumption. In these trials, patients are explicitly told they are receiving a placebo (like a sugar pill) that contains no active medication. Surprisingly, many patients still experience significant symptom improvement.[2]
This phenomenon relies on expectancy learning. When a doctor takes the time to explain how the placebo effect works—describing it as a way to unlock the body's natural healing ability—the ritual of taking a pill can still trigger the brain's relief pathways. The context, the care, and the ritual itself tell the brain that “help is on the way,” initiating the biological response without the need for lying.

The Nocebo Effect and the Biology of Empathy
The mind’s power to influence the body is a double-edged sword. The same mechanisms that drive the placebo effect can trigger the nocebo effect, where negative expectations induce actual physical harm or worsen symptoms.[6]
If a patient fears a treatment or feels dismissed by their doctor, their anxiety can activate neurobiological pathways that amplify pain perception. This reality elevates the role of the physician beyond that of a mere technician. A doctor’s empathy and communication style are active biological interventions.[2] By fostering trust and setting positive expectations, healthcare providers are not just being polite; they are chemically priming the patient’s brain for recovery.

Redefining Healing
As neuroscience continues to decode the mechanisms of top-down cognitive control,[4] we are moving toward a future where the mind is recognized as a primary architect of recovery. The placebo effect is not a trick to be eliminated, but a powerful tool to be harnessed. By understanding the biology of belief, we can better appreciate how context, ritual, and expectation shape our physical reality.
