When we check a clock, we assume time is a steady, objective backdrop to our lives. But neuroscience reveals that what we experience as the “now” is actually a complex, active construction by the brain. On the latest episode of Psych Class, we explored how this delicate process functions and, crucially, how it fractures in conditions like schizophrenia.
Listen to the episode
The Illusion of Control: Temporal Perception and Schizophrenia
The Brain’s “Now” Window
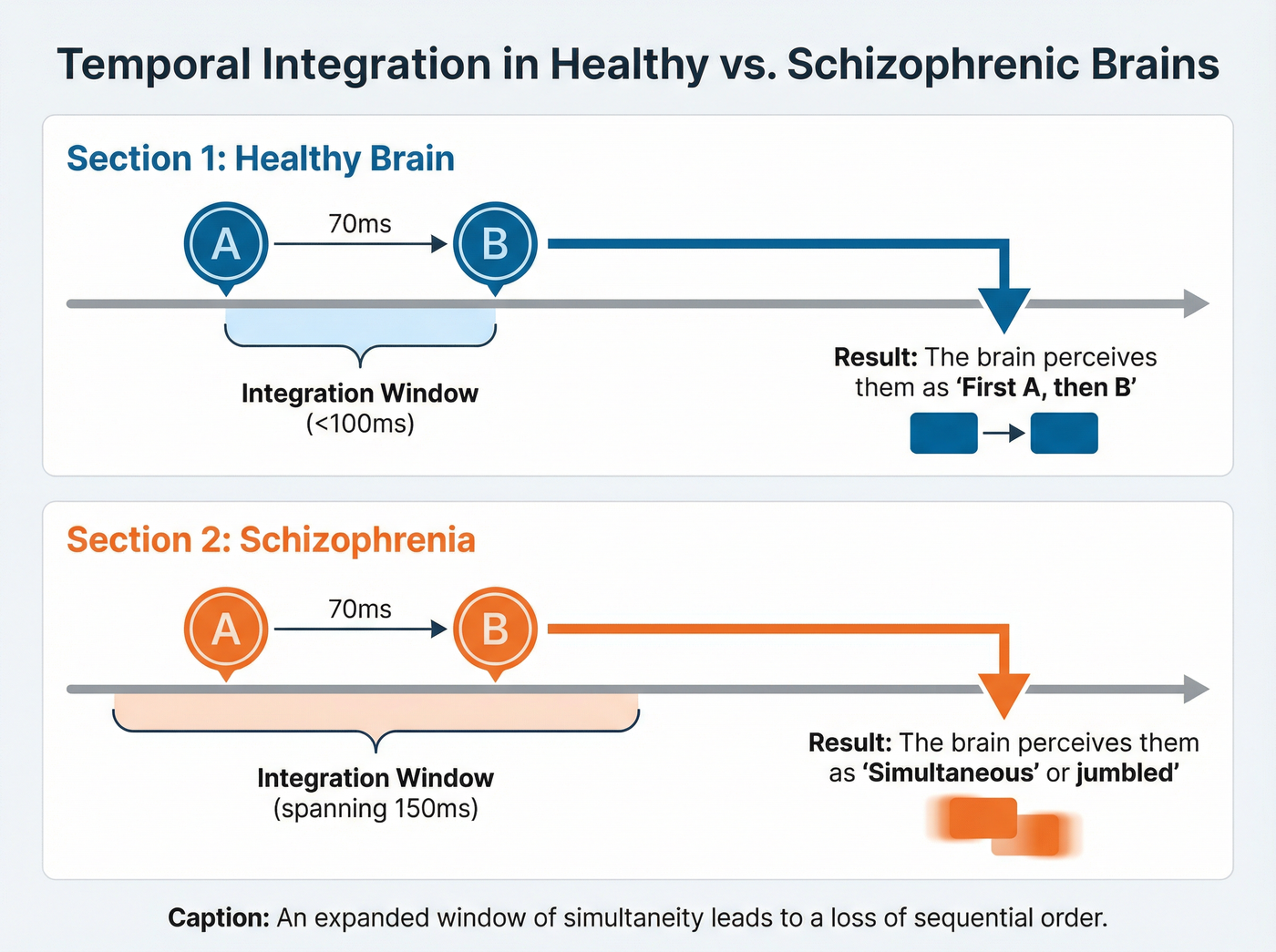
Our perception of a continuous reality relies on a process called temporal integration. The brain does not process every photon of light or sound wave instantly. Instead, it operates with a critical time window, estimated to be between 50 to 100 milliseconds. Within this brief span, the brain actively combines various sensory inputs—like sight and sound—to create a unified experience.[1]
For example, when you see someone’s lips move and hear their voice, these signals arrive at your brain at slightly different times. Yet, thanks to temporal integration, you perceive them as a single, synchronous event. This tight control is essential for maintaining a stable sense of reality.
When the Window Breaks Down
In individuals with schizophrenia, this seamless flow can splinter. Historical accounts by psychiatrists like Minkowski described patients experiencing an “absence of the feeling of duration,” where time itself seemed to stop moving forward. Modern research supports this, indicating that the window of simultaneity in these patients can become unusually large or “stuck.”[3]
When this window expands, events that are objectively separate might be perceived as happening at distinct times, or conversely, events that should be separate blur together. This leads to a fragmented experience where the sequence of reality becomes scrambled. A patient might struggle to determine the order of events in a conversation or perceive sounds as occurring “inside” visual events incorrectly.
Recent studies utilizing the “Attentional Blink” paradigm have shown that patients with schizophrenia exhibit increased temporal integration deficits within a hundred-millisecond timescale. Importantly, this issue is distinct from general attention deficits; it is a fundamental problem with how the brain binds moments together.[5]
The Neural Neighborhoods of Time
Contrary to the idea of a single “master clock,” the brain employs a distributed system for processing time. Research identifies clear functional distinctions between different types of timing:[3]
- Temporal Order Processing: The ability to judge which event happened first (A before B). This preferentially engages the left inferior parietal cortex.
- Duration Estimation: The ability to measure how long an event lasts. This recruits a circuit involving the basal ganglia, cerebellum, and supplementary motor area.
In schizophrenia, the connectivity between these regions—specifically from the right dorsolateral prefrontal cortex to the inferior parietal lobe—appears to be disrupted. This temporal dysconnectivity suggests that the disorder is not just about chemical imbalances like dopamine dysregulation, but about a failure in the brain's timing architecture.
A New Perspective on Symptoms
Understanding these timing deficits offers insight into the positive symptoms of schizophrenia, such as hallucinations. If the brain fails to accurately predict when a sound should occur in relation to a person's own movement, they may attribute their own inner voice to an external source. This failure of the “forward model”—the brain's ability to time-stamp its own actions—creates a terrifying disconnect from the self.
As research from 2024 and 2025 continues to bridge the gap between aberrant time processing and cognitive dysfunction, we move closer to viewing these timing issues not just as side effects, but potentially as core features of the condition.[1]
Sources
- Bridging the gap between aberrant time processing and cognitive dysfunction in schizophrenia: a potential core feature? | Schizophrenia
- The distinction between temporal order and duration processing, and implications for schizophrenia
- Temporal perception deficits in schizophrenia: integration is the problem, not deployment of attentions | Scientific Reports
